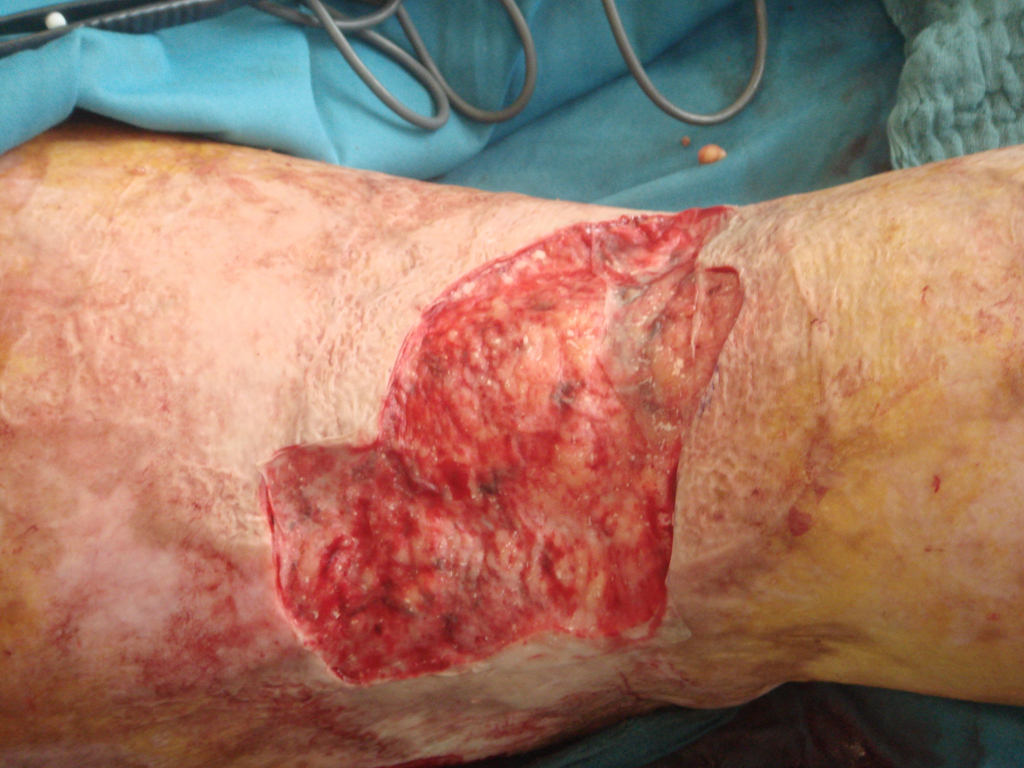
Indications
When dermal structures are preserved, split-thickness skin grafting is sufficient to achieve definitive wound closure. However, for full-thickness skin defects with loss of the dermis, split-thickness skin grafts are suboptimal. To replace the dermis, full-thickness skin or collagen-based dermal substitutes can be transplanted. However, full-thickness skin grafting can only be applied to small areas because of the limited donor area or must be expanded by complex expanders in multiple procedures.
SkinDot solves this problem. Through the SkinDot technique, all skin layers including skin appendages are transplanted in the form of 1-3 mm autologous full-thickness skin islets. Thus, epidermal and dermal skin layers are implemented into the wound. For which indications SkinDot is suitable, you can read here on this page.
Indication IIb° – III° burn
While IIa° thermal lesions heal spontaneously due to pluripotent stem cells preserved in the dermis and subcutaneously by transmission into keratinocytes, IIb° – III° burns and premature lesions require surgical treatment. Thus, Jack-Louis Reverdin performed the first autologous skin transplantation as early as 1872. He used split skin grafts of approx. 2 cm² in size, which had central dermal portions. Work on full-thickness skin grafting can be found in Davis, who transplanted full-thickness skin islets as small as 2-3 mm into a wound in the early part of the century.
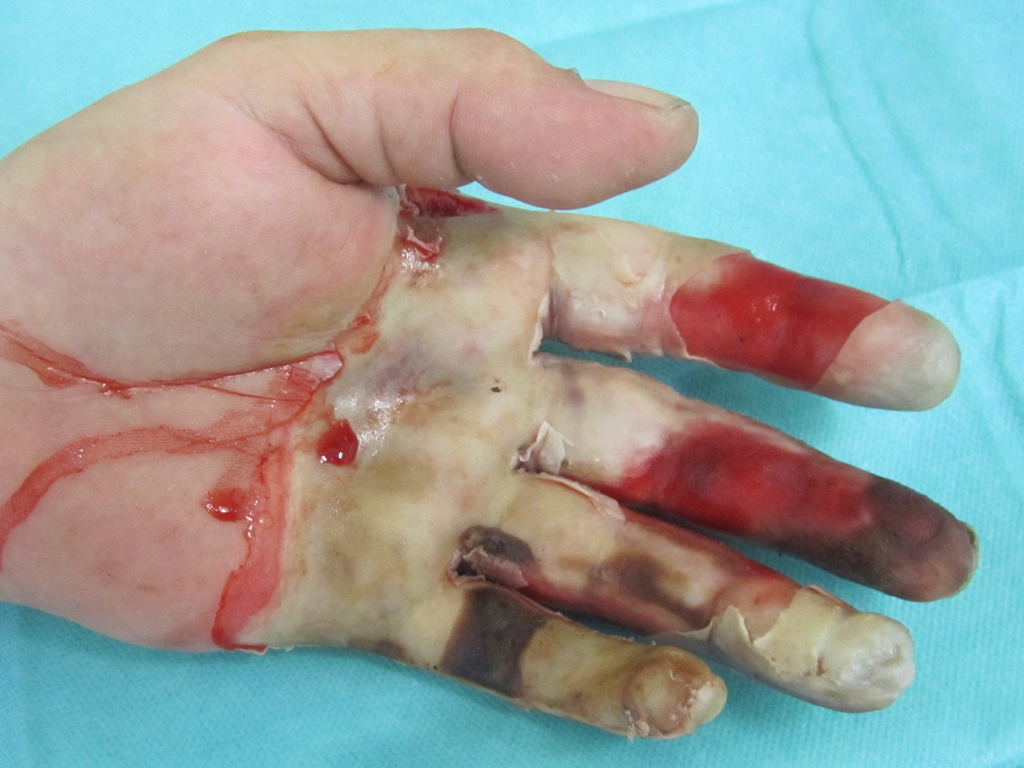
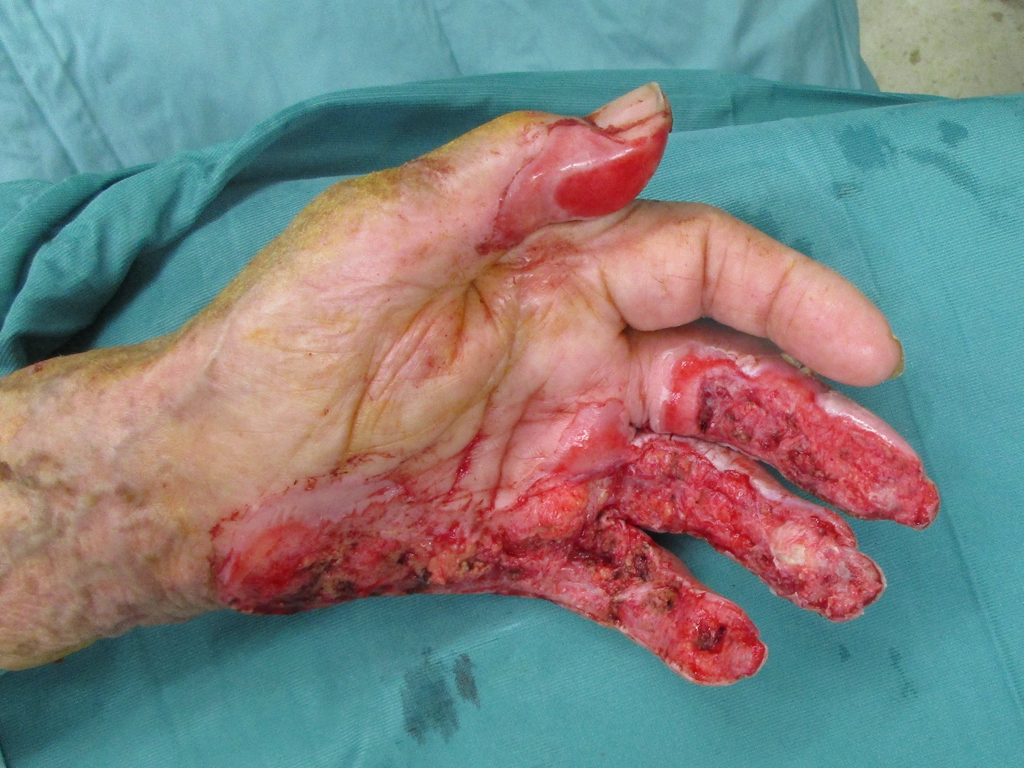
Full-thickness skin has been required mainly in mechanically stressed regions such as the palms of the hands and soles of the feet. Autologous full-thickness skin is otherwise rarely transplanted in acute care for small, third-degree burn defects, but is mainly used in the reconstructive treatment of burn sequelae (e.g., scar contractures or amputation stump care)
.
The main disadvantage of autologous full-thickness skin transplantation is the limited donor area. The advantages of full-thickness skin graft are optimal skin quality because all skin appendages such as sweat glands, sebaceous glands, nociceptors (for pain, heat, cold, pressure and vibration) are included including pluripotent stem cells. In addition, the full-thickness skin graft has little tendency to contract. A stable, resilient full-thickness skin graft with a dermal shift layer results.
.
The problem of limited availability of full-thickness skin grafts is solved by SkinDot. With the new, innovative SkinDot full-thickness skin grafting method, a surgical procedure is now available for the first time in which ubiquitous full-thickness skin donor sites can be used from the entire body by harvesting and transplanting 1 – 3 mm full-thickness skin islets. Thus, a large-area full-thickness skin equivalent is available without limitation in the acute treatment of deep thermal lesions.
Indication acute wounds
Bei akuten tiefen Wunden ersetzt das SkinDot Verfahren die komplette Haut durch das Vollhautäquivalent, einschließlich der darin enthaltenden Hautanhangsgebilde.
So wird die natürliche Funktion gesunder Haut wiederhergestellt. Akute Wunden sind definiert als plötzliche, meist durch einen Unfall entstandene Verletzungen von zuvor ungeschädigter Haut und Gewebe. Abhängig von ihrem Entstehungsmechanismus werden mehrere Arten von akuten Wunden unterschieden:
Risswunden: (Vulnus Lacerum)
Risswunden werden meist durch grobe Klingen von Kreissägen oder Fräsen verursacht. Sie zeichnen sich durch zerfetzte Wundränder aus und enthalten viele tote Gewebeanteile. Komplizierend treten häufig Verletzungen von Sehnen, Nerven oder anderer funktionalen Strukturen auf. Die Wundränder müssen meist neu angeschnitten und mittels Hautnaht versorgt werden. Nur wenn die Wundränder nicht spannungsfrei genäht werden können, ist eine Hauttransplantation notwendig.
Quetschwunden (Vulnus Contusum)
Die durch stumpfe Gewalteinwirkung entstehende Quetschwunde zeichnet sich durch tiefe Wundtaschen mit zerfetzten Wunderändern aus. Die Wiederherstellung des zerstörten Gewebes ist meist unmöglich. Tote Gewebeanteile müssen entfernt werden und das lebende Gewebe durch Naht und/oder eine Hautverpflanzung versorgt werden.
Crack-squeeze wounds (Vulnus Lacero-Contusum)
In the case of laceration-crush injury, there is usually no isolated accidental mechanism, but a combination of several forces acting on the tissue. Lacerations are often caused by the action of high blunt force. Due to the combination of compressive, impact, and tensile forces, the wound edges are usually irregularly lacerated and bloodshot. Radical surgical debridement is required for treatment, and the wound edges must be re-cut and sutured. If tissue tension is too high to allow wound closure by suturing alone, skin must be transplanted.
Lacerations (Vulnus scissum)
Lacerations are caused by sharp objects such as kitchen knives, razor blades or glass splinters. The wound edges are smooth and only slightly gaping. They tend to bleed profusely and can usually be treated – after wound cleansing – by suturing the skin. Careful assessment of symptoms can estimate the extent of damage to deep-seated structures. In the case of deep wounds and the possible presence of foreign bodies, surgical wound cleansing (debridement) is often performed before wound closure in the case of incised wounds.
Scrapes (Excoratio)
This superficial injury to the skin is caused by friction against rough surfaces, e.g. in a bicycle fall. Blood loss from these wounds is usually minor, but the often severe contamination requires thorough surgical cleaning. Skin suturing or skin grafting is not necessary.
Decolllement
Decollement is a special case of the abrasion wound. Due to tangentially acting shear forces, parts of the skin or the entire skin detach and large wound areas develop. The cause is usually rollover trauma in the context of traffic accidents or severe motorcycle crashes at high speeds. In the case of decollement, skin grafting is always necessary.
Stab wounds (Vulnus Ictum)
Stab wounds are characterized by mostly small puncture sites, which means that the extent of internal injuries is often underestimated. For this reason, careful exploration of the deep tissue is absolutely necessary in this type of wound.
Bite wounds (Vulnus morsum)
A bite wound is usually a combination of puncture, crush and laceration wounds with the risk of microbial contamination by the saliva of the causer. A peculiarity in the care of these wounds is that they have been treated openly for centuries, i.e. wound care by suturing was obsolete. Only with the new and safe antibiotics can bite wounds be treated by suturing. This is mainly done for bite wounds on the face of children. Bite wounds can have very small wound openings, but often have a considerable depth.
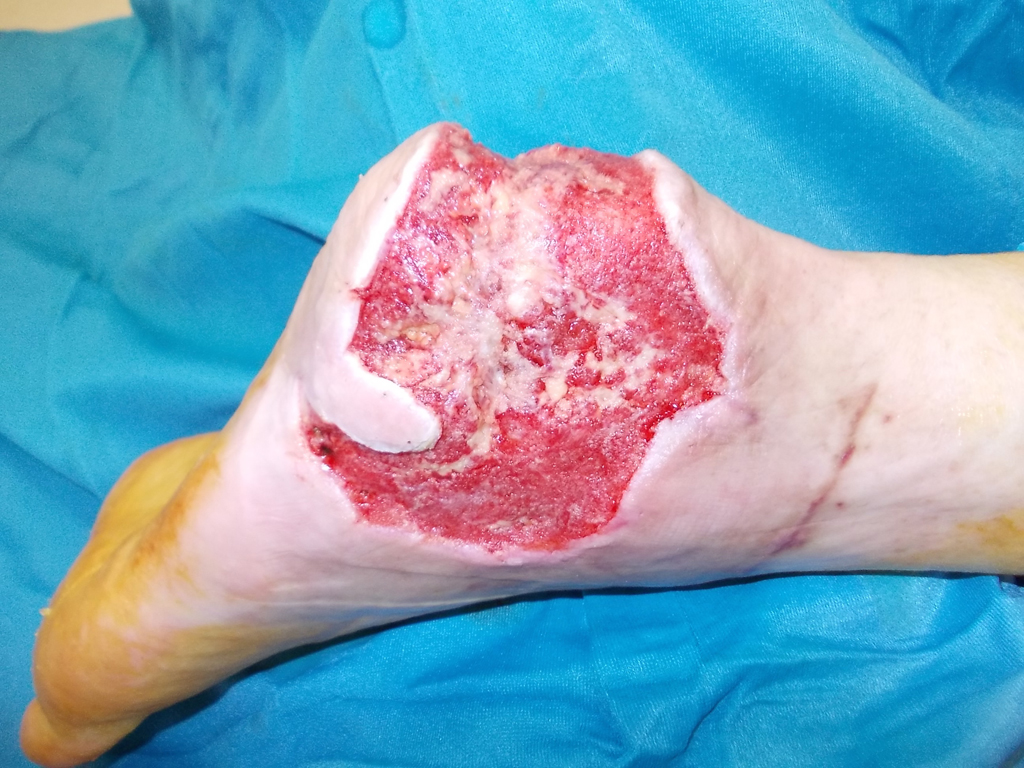
In acute wound care, SkinDot is particularly suitable for full-thickness skin defect wounds in the face, on the hands and feet, and over joint surfaces. Since the SkinDot procedure results in a stable full-thickness skin substitute, amputation stumps can be treated with the SkinDot graft in primary care. The SkinDot skin substitute is also particularly suitable for large decollement injuries.
Indication – Chronic wounds
Wound healing is a complex physiological process that should be completed as undisturbed as possible. Wounds without a tendency to heal over a period of three months are defined as chronic wounds. Chronification occurs on the ground of pathological tissue conditions.
In Germany alone, there is a 2% prevalence of chronic wounds with severe losses in patient quality of life. There are annual costs of about 8,000-10,000 euros per patient due to the failure of wound closure. The most common causes are leg ulcers, decubitus ulcers and diabetic ulcers. The acute wound heals without major therapeutic intervention as part of the concerted temporal progression of the physiological wound healing phases, these are the inflammation-proliferation, regeneration, and remodeling (maturation) phases.
The pathophysiology of wound chronification is very heterogeneous (e.g., due to diabetic metabolism, pressure ulceration, venous stasis ulceration). As conditions, a wound bed before skin grafting should have good vascularization, be free of debris and avital tissue, and contain freedom from infection and moderate moisture. Effective, rapid wound closure can only be achieved with skin grafting. However, in chronic wounds, results after split-thickness skin grafts are often frustrating because the thin split-thickness skin graft does not contain a dermal shifting layer, resulting in a stiff skin substitute.
The SkinDot procedure transplants full-thickness skin into the chronic wound, preventing multiple reoperations. Through SkinDot, the often massive reduction in quality of life caused by the chronic wound can be significantly improved by a single surgical procedure. The high annual treatment costs are significantly reduced by the definitive wound closure.
Indication – scar correction
If the number of regenerative skin cells (stem cells) in a wound is too low, the healing process is delayed. Originally healthy tissue is replaced by the body with defect tissue as part of the wound healing process. This inferior defect tissue is called scar tissue. Scar tissue is inelastic, lacks physiological skin functions such as sweat or sebaceous gland secretion, and therefore tends to be dry and vulnerable.
When scars are cosmetically noticeable, patient distress can be very high, especially with stigmatizing scars on the face, forehead, décolleté, or back of the hand. Regardless of appearance, scars lead to functional limitations, especially if they are located over joint surfaces and lead to restricted movement. A special form of scar is the so-called “hypertrophic” scar. According to studies, the duration of wound healing correlates with the occurrence of hypertrophic scars. Wounds that do not heal completely within 21 days therefore show a tendency to scar hypertrophy. Surgical scar therapy in the context of reconstructive treatment represents a classic indication for a full-thickness skin graft. SkinDot is a new, innovative procedure that replaces scar tissue with full-thickness skin grafts. After the SkinDot procedure, the transplanted skin layers confluence to form a full-thickness skin equivalent, resulting in a stable and resilient graft.
Do you want to offer the new, innovative SkinDot procedure to your patients? Contact us! We support you with joint surgery planning, surgery execution, matrices, and corresponding patient documents (informed consent form, risk exclusion). We look forward to hearing from you!
Skin Transplantation beyond
Skin Transplantation 2.0